What is sleep apnea?
Sleep apnea is a serious sleep disorder that occurs when there is the absence of inspiratory airflow for at least 10 seconds causing irregular/broken breathing patterns. This results in drop in oxygen saturation in the blood being circulated in the body.
What are the types of Sleep Apnea?
- Obstructive Sleep Apnea (OSA): This is the most type of apnea. In OSA the throat muscles relax causing obstruction in normal breathing.
- Central Sleep Apnea (CSA): In CSA the brain doesn’t send proper signals to the muscles that control breathing.
- Complex sleep apnea syndrome: This type of apnea is a mixture of both obstructive sleep apnea and central sleep apnea.
- Hypopnea: Another variation of apnea is Hypopnea which is a result of abnormally slow or shallow breathing.
What are the major risk factors for sleep apnea?
Some of the major risk factors for apnea are – obesity, old age, large neck size, nasal obstruction due to allergies or sinus. If left untreated, sleep apnea can increase the risk of health problems such as – high blood pressure, stroke, heart failure, diabetes, depression, worsening of ADHD, and headaches.
Undiagnosed OSA is also associated with an increased likelihood of hypertension, cardiovascular disease, stroke, daytime sleepiness, motor vehicle accidents, and diminished quality of life. It is found that OSA had 80% comorbidity with other lifestyle diseases. Studies have also shown that Obstructive sleep apnea (OSA) has the highest prevalence, from 13% to 33% in men and from 6% to 19% in women.
What is the conventional method to detect apnea?
AHI is determined by a Polysomnography (PSG) test which is performed overnight on subjects in a resource-intensive specialized sleep center which require the subjects to wear encephalography (EEG) electrodes, oronasal airflow sensors, thoracic and abdominal respiratory inductive plethysmography (RIP) belts, electrocardiography (ECG) sensors, an oxygen saturation finger-clip sensor, a body position sensor, chin and leg electromyography and electrooculography sensors over a full night.
How is it assessed?
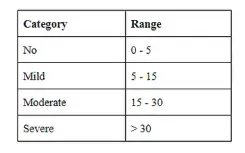
Sleep apnea is generally assessed by the Apnea-Hypopnea Index (AHI) which is the number of apnea and hypopnea episodes per hour.
The below table shows the classification of subjects based on AHI:
How do we determine AHI?
We determine AHI using Dozee that captures data pertaining to movements(pressure/pulses) caused by heartbeats and respiration.
This method just requires the subject to place the Dozee mat under the mattress below the chest(thorax) region overnight. The data obtained is processed and a respiratory signal is obtained using which AHI is calculated.
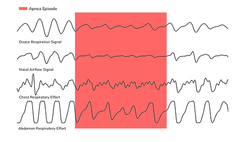
The below image shows how an apnea episode looks life over various signals.